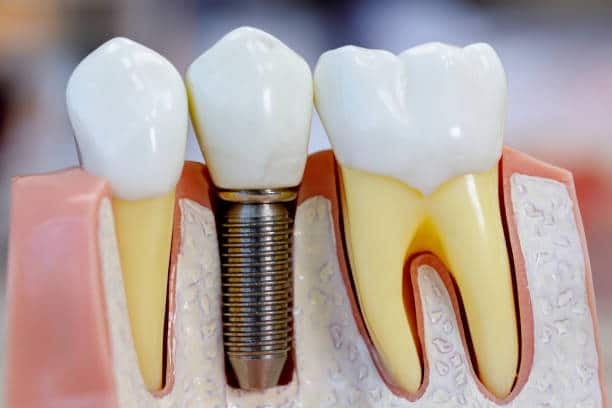
Dental Implants for Diabetics: What You Need to Know
Introduction
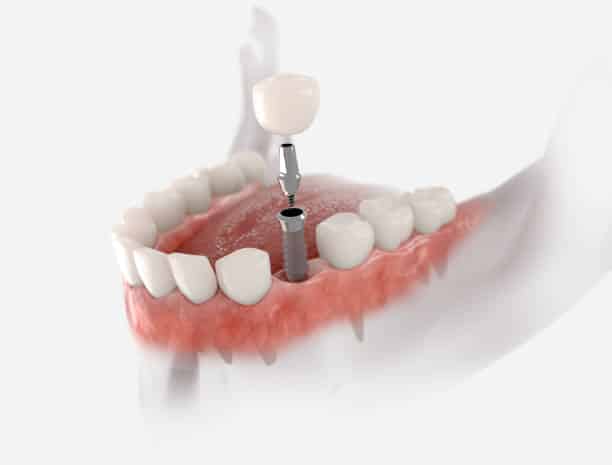
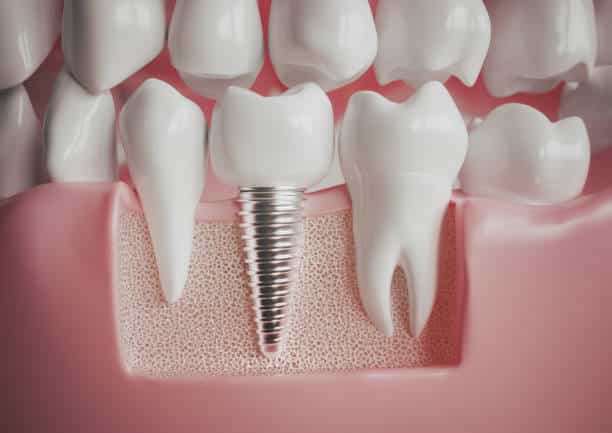
Dental implants have revolutionized the field of dentistry, offering a durable and natural-looking solution for replacing missing teeth. However, for individuals with diabetes, considerations regarding oral health and dental procedures become even more crucial. This article explores the unique challenges and important considerations surrounding dental implants for diabetic patients. For more Information regarding dental implants consult our Dentist Plano.
Understanding the Impact of Diabetes on Oral Health
Diabetes can have significant implications for oral health, increasing the risk of gum disease, tooth decay, and oral infections. Poorly controlled blood sugar levels can compromise the body’s ability to fight bacteria, leading to more severe oral health issues. Therefore, individuals with diabetes must maintain meticulous oral hygiene practices and undergo regular dental check-ups to prevent complications.
Assessing Candidacy for Dental Implants
Before proceeding with dental implant surgery, diabetic patients must undergo a thorough evaluation by their dentist or oral surgeon. Factors such as blood sugar control, overall health status, and bone density are taken into consideration to determine candidacy for implants. Poorly controlled diabetes or underlying medical conditions may increase the risk of complications and impact the success of the implant procedure.
Importance of Blood Sugar Control
Blood sugar control is paramount for diabetic patients undergoing dental implant surgery. Elevated blood sugar levels can impair wound healing and increase the risk of postoperative infections. Dentists often collaborate with patients’ healthcare providers to optimize blood sugar levels before and after implant surgery, ensuring a favorable outcome and minimizing the risk of complications.
Preparing for Implant Surgery
Prior to implant placement, diabetic patients may undergo additional pre-operative assessments and precautions to mitigate risks. This may include antibiotic prophylaxis, meticulous oral hygiene instructions, and modification of medication regimens. Patients are advised to disclose their diabetes status and any related medications or complications to their dental care team to facilitate personalized treatment planning.
Managing Post-Operative Care
After dental implant surgery, diabetic patients must adhere to strict post-operative care guidelines to promote optimal healing and implant integration. This may involve regular monitoring of blood sugar levels, adherence to prescribed medications, and avoidance of smoking or alcohol consumption, which can impede healing. Any signs of infection or delayed healing should be promptly reported to the dental provider for timely intervention.
Long-Term Oral Health Maintenance
Long-term success of dental implants in diabetic patients hinges on diligent oral hygiene practices and regular dental follow-ups. Patients are encouraged to maintain a healthy lifestyle, including a balanced diet, regular exercise, and routine dental cleanings to prevent complications such as peri-implantitis (inflammation around the implant). Close collaboration between the dental and medical care teams is essential to ensure comprehensive management of diabetes and its impact on oral health.
Conclusion
Dental implants offer a transformative solution for restoring function and aesthetics in individuals with missing teeth, including those with diabetes. However, successful implant treatment requires careful consideration of the unique challenges posed by diabetes and meticulous management of blood sugar levels before, during, and after surgery. By prioritizing oral health and maintaining open communication with healthcare providers, diabetic patients can enjoy the benefits of dental implants while minimizing the risk of complications.